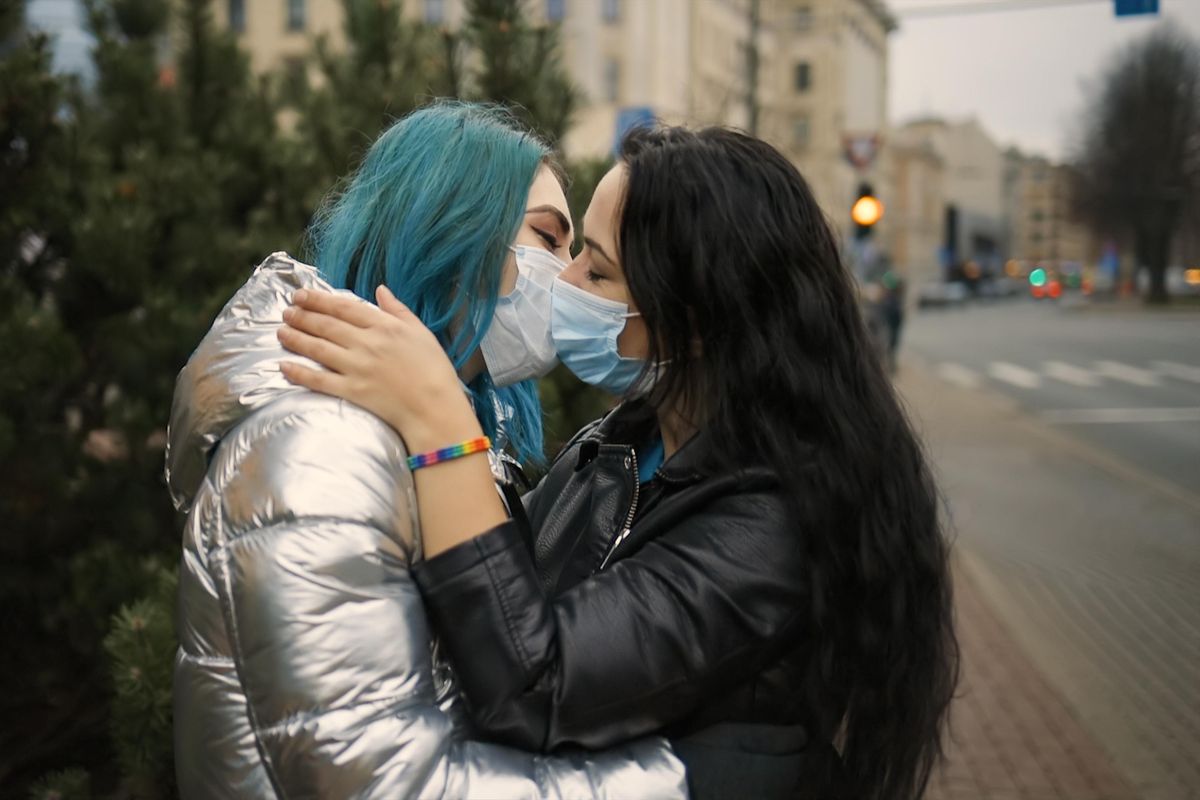By Tamra Burns Loeb, University of California, Los Angeles; Gail Wyatt, University of California, Los Angeles, and Michele R. Cooley-Strickland
With college students back on campus, and COVID-19 with us for the foreseeable future, it has become increasingly clear that educators need to develop a new definition of safer sex.
Although the virus is not a sexually transmitted infection, students can spread COVID-19 through droplets and particles, especially when within 6 feet of each other. That includes being intimate.
This is why sex education efforts need to inform students not only about sexually transmitted infections, HIV and unintended pregnancy, but also about ways to reduce COVID-19 transmission risk.
As psychologists and educators at the University of California, Los Angeles, who design interventions to promote the health and well-being of college students, we are aware of the work that has gone into reopening campuses during the pandemic. But despite all the effort, some critical health needs of those students have been entirely overlooked.
The CDC missed a chance
The Centers for Disease Control and Prevention produced a lengthy document, last updated in November 2021, about college campuses and COVID-19 transmission. The document offers suggestions on how to stop the spread of the virus in all kinds of scenarios, from communal eating to sporting events. But stunningly, we could not find a word about the potential for spreading COVID-19 within an intimate relationship.
This is particularly disturbing when one considers that college students could use some expert advice. Their decision-making skills are not fully developed, and many college-age students are impulsive.
Pleasurable and perhaps risky behaviors often win out over possible long-term negative consequences. Just look at the rates of STIs, HIV and unintended pregnancy: Compared with other age groups, the rates are higher among college students.
Ways to avoid COVID-19
The irony is that there is much to say and to promote about reducing COVID-19 risk for sexually active students.
Here are some evidence-based recommendations: Limit the number of sexual partners. Avoid sexual contact with anyone who has COVID-19 or symptoms. Use condoms and dental dams. Avoid activities involving transmission of fecal-oral material. Wear masks during intimate acts. Avoid kissing.
Also: Wash hands before and after sexual activity. Use clean sex toys. Sanitize areas where sexual activity occurs. Engage in self-pleasure. And understand that those who are not symptomatic can still transmit COVID-19 and some STIs.
Abstinence programs don’t help
Many abstinence programs are based on the premise that abstinence until marriage is the acceptable standard of human sexual behavior.
But research has shown that abstinence programs are ineffective and often lead to increased rates of unintended pregnancy and other high risk behaviors. That’s because they limit discussions of STI prevention and birth control; this effectively withholds information from young people who are in the midst of making crucial decisions about their health and future.
Instead, research shows that programs that provide accurate information in a nonjudgmental way about abstinence, contraception and STI prevention work better, particularly if they also promote communication, decision-making and negotiation skills.
These same programs could also add information about preventing the spread of COVID-19 while sexually intimate.
How schools can help
Instead of ignoring the issue, university administrators should make sure students have the tools they need to avoid both COVID-19 and STIs.
For example, with just their smartphones, students can easily schedule COVID-19 tests, get the results and then share them with those they are intimate with. The same can be done with STI, HIV and pregnancy results.
Sharing those results with respect for confidentiality requires widespread promotional campaigns to normalize this new behavior. Schools or campus-based student organizations could ignite a trend on Twitter with a simple but memorable slogan. Here’s one we suggest: “Show me yours and I’ll show you mine.” That’s one of many Twitter-friendly lines that would encourage students to exchange electronic health records.
Some campuses already have vending machines that contain free COVID-19 self-test kits. Results are sent to students electronically. At UCLA, the self-test kits are placed near sexual health vending machines, which are stocked with condoms, lubricant, emergency contraception and other reproductive and sexual aids.
Learning to interact again
Communication between students is critical, particularly when sharing intimate information. But after 18 months away from campus because of COVID-19, some have experienced serious social and emotional impacts. For many, peer-to-peer communication skills have declined. This awkwardness makes it particularly difficult when discussing sensitive subjects.
Again, the school can help. One way is to offer students breakout sessions in small groups. This could be done in-class or as extracurricular assignments. Either approach gives socially anxious students – or those recovering from COVID-19 isolation – the outlet they need to interact in person with others.
How parents can help
Young people have been bombarded with sexual misinformation from both peers and media. But studies show that intergenerational communication about sexual activity can reduce risky sexual behaviors. And while sexual health education is effective at reducing unwanted outcomes, it’s enhanced when parents are involved.
With the widespread impact of COVID-19, now is a great time to bring parents into the conversation. But they are often an underutilized resource. Many haven’t had sexual health education themselves, they may not know what’s appropriate to share with their children and they may simply be uncomfortable with sex topics.
We are still in a time of considerable ambiguity, mistrust and confusion. That applies to both COVID-19 and sexual health. But there is one certainty: Young people need responsible adult guidance to secure a healthy future. And the sooner the better. In the grip of a pandemic, their lives may depend on it.![]()
Tamra Burns Loeb, Adjunct Associate Professor, Department of Psychiatry and Biobehavioral Sciences, University of California, Los Angeles; Gail Wyatt, Dena Bat Yaacov Endowed Chair and Distinguished Professor of Psychiatry & Biobehavioral Sciences, University of California, Los Angeles, and Michele R. Cooley-Strickland, Project Scientist and Clinical Psychologist, Department of Psychiatry and Biobehavioral Sciences
This article is republished from The Conversation under a Creative Commons license. Read the original article.